Public Health in the Age of Austerity
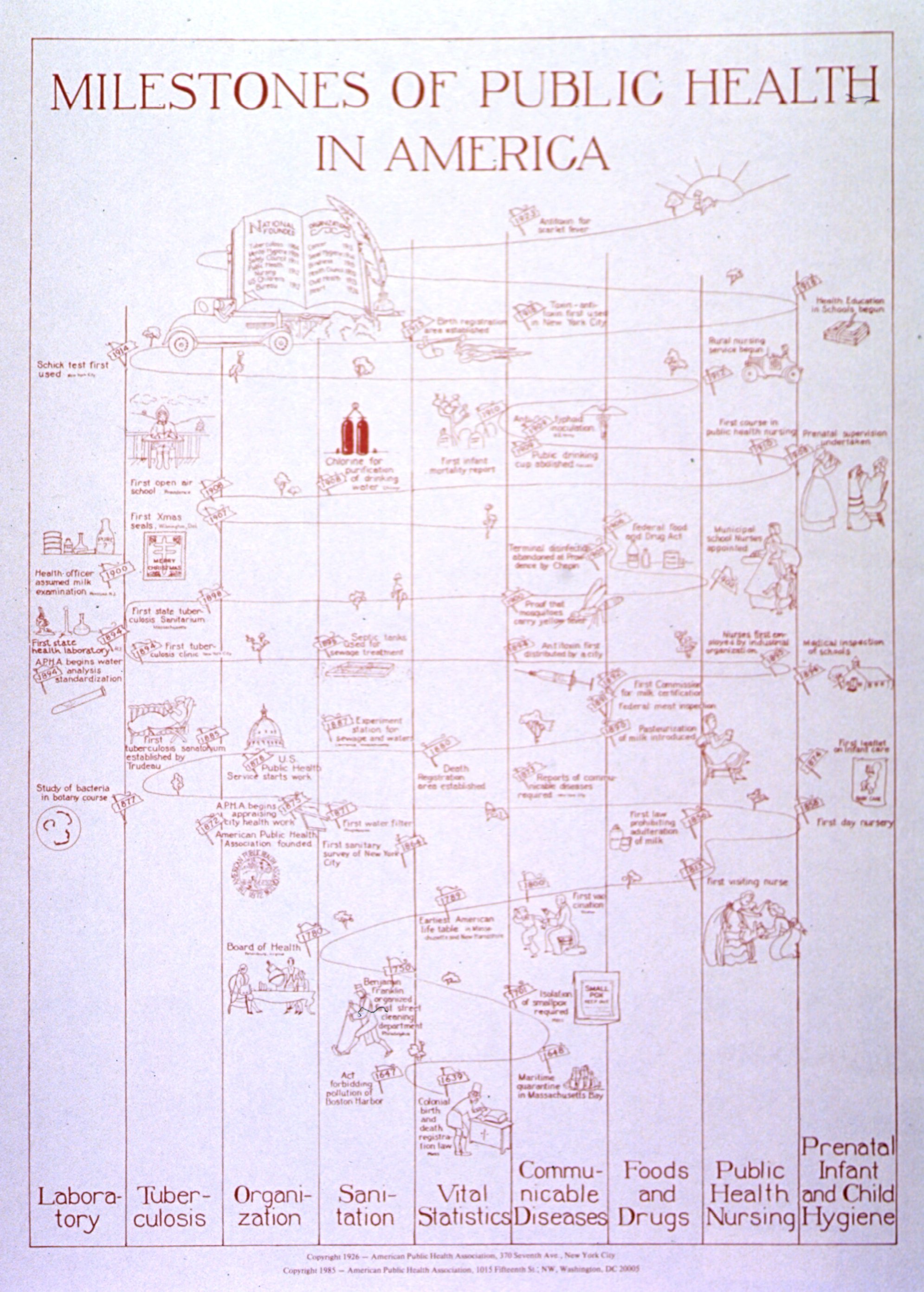
“Care of the public health is the first duty of the statesman”
In 1932, the American Public Health Association, publishing in the American Journal of Public Health, called on their government not to forget about them. The consequences, they claimed, would be dire. They described it as a present state of emergency.
At the time, they felt that the situation in the United States, during the heights of the depression, had got to such a state, that it warranted immediate action. They sought to call attention to the inherent dangers involved in slashing public health budgets, reducing personnel, and limiting health programmes. They cited preventive campaigns against diphtheria and typhoid fever that would suffer.
It was the time of the Great Depression. The decade that immediately preceded it — the roaring 20s — saw runaway economic growth providing prosperity for all. The end of the decade and the 30s, however, began to stagnate, signposted by the stock market crash of October 1929. The collapse of Wall Street was followed by a steep decline in economic activity — gross domestic product was counted in negative numbers, and unemployment was at an all-time high — reaching a historical maximum of 22.9% in the US in 1932.
The idea has always been that an economic downturn also led to a downturn in public health. Historically, there has been no greater spur of health and wellbeing than a prosperous nation. The wealthier the nation then the more it spent on the health of its citizens. It may seem counter-intuitive to think that the era of the Great Depression was a time that actually saw declining death rates in Europe and in the US. During the Great Depression, life expectancy rose significantly from 57.1 years of age in 1929 to 63.3 years in 1933. Rates of infant mortality declined during the 1920s and 1930s. Within those two decades the only years that saw an increase in mortality were years that coincided with short bursts of strong economic growth. Famously, the most notable cause of death during this period was suicide. Death by suicide peaked with unemployment.
“It is futile to quote the great men of the past, statesmen, as well as scientists, to prove what health means to any nation.”
This is a recurring theme over the course of history. One that we don’t pay much attention to. As the health of a nation gets better we tend to forget of the vigilance and strife that was needed the first time round. Eventually, health is a given. So much so that it is only when a scandal hits that we see how much we take it for granted. Comparing developed against developing nations is where we see the greatest contrast. Vaccinations are part and parcel of a newborn life in some countries. Children cannot go to school without it. This seamless integration of public health into everyday life does not exist everywhere.
Fast forward to today’s economic recession, where the US is witnessing a decline in its public health laboratories. These public health laboratories provide testing for drinking-water testing, sexually transmitted diseases, HIV screening, blood lead screening, substance abuse monitoring to support treatment programs, and detection of bioterrorism agents in environmental samples and isolates from humans.
A decline that is due in part to deficient state and local tax revenues resulting from loss of taxpayer jobs and income tax revenues and loss of homeowner and business property tax payments due to foreclosure. Decreased funding has resulted in loss of public health jobs due to layoffs and attrition, program cuts and reductions.
When the University of Michigan’s Center of Excellence in Public Health Workforce Studies, together with the Association of Public Health Laboratories, assessed the workforce and program capacity in US public health laboratories back in 2011; they found that almost half of laboratories anticipated that more than 15% of their workforce would retire, resign, or be released within 5 years.
In Michigan, they lost more than 300 years’ worth of employee experience over the course of 3 months. In attempts to control budgets, state and local governments incentivized retirement. Resulting in loss of the most experienced, expert employees and additional burden of work for remaining employees.
Cuts and straitened times seems part and parcel of today’s economic downturn. Little discussion takes place on how this will ultimately shape the health and wellbeing of nations. Demand for services from an ageing population and increased costs created by new clinical and pharmacological technologies, will all put upward pressure on health spending. This is the case in the US and in the UK.
Some see it as an opportunity, however. An opportunity to finally bring two opposing forces together — public health and medicine. Writing in the New England Journal of Medicine, researchers argue for simple population-based approaches to address fundamental health problems. Obesity tackled at the population level rather than at the individual level. A focus on the population as a whole rather than simple service delivery of intervention medicine.
“Perhaps paradoxically, the current push for austerity could bring together clinical medicine and public health in unprecedented, mutually beneficial ways that could improve population health and reduce spending”
The idea is simple and looks to do more with less. Such is life in the age of austerity.
Image — source
 Follow
Follow